Medical cover,
on the move.
Crypto-native medical cover for unexpected hospital events during an active coverage window. Two plans. Clear caps. Clear claims flow.
Contents.
- 01 What it is
- 02 The two launch plans
- 03 Payouts by tier
- 04 What's actually covered
- 05 Eligibility & controls
- 06 How to enroll & claim
- 07 What to submit with a claim
- 08 Decision timeline
- 09 Claim lifecycle
- 10 Trust & review roadmap
- 11 Reserve & capital model
- 12 Outside scope in v1
- 13 Non-goals for v1
- 14 Sponsors & cohorts
- 15 Full FAQ
- 16 Surfaces & resources
Information current as of 2026. Terms vary by series and cohort. This document is informational — refer to plan documentation for binding terms. Not medical advice.
What it is.
OmegaX Protect is crypto-native medical cover for unexpected hospital events during an active coverage window — not ongoing care, not chronic treatment, not lifestyle medicine.
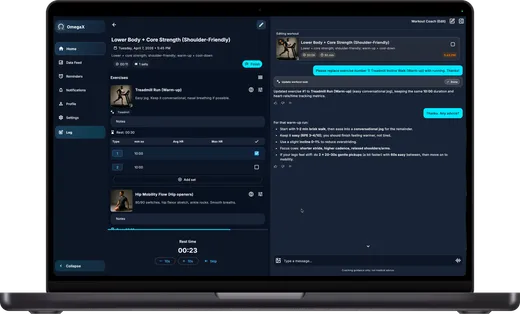
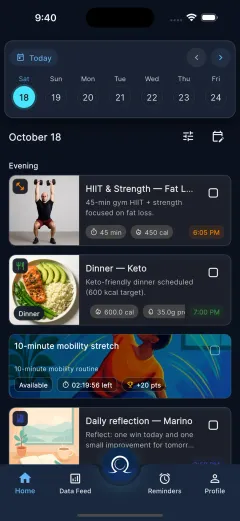
Members use the OmegaX app to enroll, verify eligibility, submit claims, upload evidence, and track status. The protocol handles the economically important state — reserves, claim status, obligations, payouts — while sensitive medical documents stay offchain.
The result is a simpler, more transparent cover layer for travelers and wallet-native teams. It is intentionally narrow in v1: one clear emergency-travel story, one visible claims flow, one reserve truth model.
The two launch plans.
One tuned for short event and offsite weeks. One tuned for longer travel and cohort programs.
Protect Event 7
Short-window protection for conference weeks, hackathons, and team offsites.
- Hospital emergencies only
- Pays a fixed amount per claim
- One claim per coverage window
- Built for conference and offsite weeks
Protect Travel 30
Longer coverage for nomads, residencies, and extended travel.
- Fixed payout plus reimbursement top-up
- One claim per coverage window
- Team pricing from 79 USDC at volume
- Built for longer travel and team programs
Launch pricing and caps shown are expected values for V1 series. Program availability, eligibility, and final terms vary by series and cohort.
Payouts by tier.
Three tiers based on what actually happened to you. Each plan pays a fixed USDC benefit on an approved claim. Protect Travel 30 also reimburses extra documented costs above the fixed benefit, up to the cap.
- Tier 1 150 USDC Verified ER or urgent hospital evaluation
- Tier 2 500 USDC Verified overnight hospital admission
- Tier 3 1,500 USDC Verified surgery, ICU, or extended admission
- Tier 1 250 USDC Verified ER or urgent hospital evaluation
- Tier 2 1,000 USDC Verified overnight hospital admission
- Tier 3 2,500 USDC Verified surgery, ICU, or extended admission
Tier is determined by the actual medical event as validated from the discharge summary, physician note, and invoice. Only one primary claim case is supported per active coverage window in v1.
What's actually covered.
A narrow, well-scoped surface: the things that actually send a traveler to a hospital without warning.
- Fracture or dislocation
- Appendicitis
- Severe dehydration or gastroenteritis requiring ER
- Acute infection requiring hospital treatment
- Sudden respiratory events requiring urgent care
Eligibility & controls.
OmegaX Protect is built to stay honest. Waiting periods, a short health attestation, and identity-bound membership keep pricing fair and reserves healthy — so the people who actually need cover get paid.
Enroll before the window starts
Coverage must be active before the trip, event, or cohort period begins. No backdated enrollment.
24-hour accident waiting period
Accident cover activates 24 hours after enrollment to prevent instant adverse selection.
7-day illness waiting period
Illness cover activates after a 7-day waiting period. Pre-approved sponsor cohorts can waive.
One primary claim per window
Each active coverage window supports one primary claim case per member in v1.
Identity-bound member position
One wallet identity and one legal identity per covered member. No shared enrollment.
Eligibility self-attestation
At purchase, member confirms they are not currently hospitalized and not seeking coverage for an already-known live event.
How to enroll & claim.
From enrollment to payout, every step runs through OmegaX. The protocol tracks settlement state underneath.
Purchase or activate coverage in OmegaX before the trip, event, or cohort window begins.
Accident cover starts after 24 hours. Illness cover starts after 7 days. Pre-approved sponsor cohorts can have adjusted windows.
File a claim in OmegaX with the required evidence — invoice, discharge summary, physician note, and proof of payment where needed.
Claims move through review, approval, and payout states. Status is visible to the member throughout.
What to submit with a claim.
Clear evidence makes fast payouts possible. Upload documents once in the app — the protocol records only references, never raw medical data.
- 01 Proof of enrollment. Confirmation that coverage was active at the time of the covered event.
- 02 Identity match. Wallet and legal identity linked to the member position on the protocol.
- 03 Proof of covered location & dates. Evidence that the event occurred inside the active coverage window.
- 04 Hospital or clinic invoice. Itemized invoice from the treating facility, with dates and services.
- 05 Discharge summary or physician note. Clinical document describing the acute event and treatment performed.
- 06 Diagnostics or prescription records. Imaging, labs, or prescribed medications tied to the covered event (where relevant).
- 07 Proof of payment. Required when claiming reviewed reimbursement top-up above the fixed benefit.
Decision timeline.
Targets for acknowledgment, review, payout, and appeal. Members see status updates in OmegaX at every step.
Timelines assume evidence is complete. Incomplete submissions re-enter review once the missing items are provided. Complex or cross-border claims may require additional review time.
Claim lifecycle.
Every claim moves through a defined set of states. Status is visible to the member throughout and anchored to the protocol for settlement.
Member files the claim in OmegaX with structured evidence.
AI claim processor runs first-pass review; operator adjudicator validates or overrides where needed.
Decision published to the protocol with a hash of the review trace for auditability.
Approved payouts create an explicit obligation on the plan reserve.
USDC is paid to the member’s payout destination. Obligation is closed.
Claim record finalized. Appeal window remains open for 7 days.
Every approved claim is set aside in the reserve before payout. Paying you out clears that hold. Denied claims release the hold back into the reserve.
Trust & review roadmap.
The app handles the human journey. The protocol handles the money. Review moves from concierge-assisted, to AI-led with human override, to decentralized operators.
OmegaX app handles the member journey
Onboarding, eligibility checks, claim intake, evidence upload, and status updates all happen in the app.
Protocol handles economic state
Reserve logic, claim status, obligations, and payout settlement live on the protocol — shared truth, not a private ledger.
AI claim processor leads review
AI oracles lead claim adjudication with operator fallback during early bootstrap. Evidence is checked against plan rules.
Sensitive data stays offchain
Raw medical records and personal health data never go onchain. Only hashes, references, and financial settlement data cross the boundary.
Bootstrap
OmegaX Health acts as the first claims-oracle surface with a concierge-assisted review layer. Members interact through the app. Decisions are written to the protocol.
AI-led with human override
AI claim processor produces the first-pass recommendation for tier detection, evidence validation, and fraud flags. Human operator override remains available during ramp-up.
Decentralized operators
Explicit decentralized claims operators, oracle set, and governance-visible dispute pathway. Review becomes transparent, auditable, and verifiable.
Your medical records never go onchain. The protocol only sees claim status, what's reserved, and what gets paid out. Full technical model in the protocol docs.
Reserve & capital model.
Payouts come from explicit, posted capital. One reserve kernel with visible lanes. No hidden liabilities, no blending of app SaaS with claims economics.
OmegaX app membership
Monthly or annual consumer subscription covering the AI health agent, data sync, voice accountability, and premium app features. Separate from claims reserves.
Protection premium
Paid per active coverage window or funded by a sponsor on behalf of a cohort. Activates protection eligibility. Can auto-renew for continuing travelers.
Member premiums
Retail and cohort premiums flow directly into the plan reserve for the active series.
Sponsor backstop
Sponsor-funded capital deposited explicitly to cover a cohort. Reserve attribution stays visible per program.
LP allocation capital
Senior open class provides stable-yield reserve. Junior first-loss class absorbs early impairment with a higher fee share. Class separation is part of the core capital design.
Protocol or ecosystem backstop
Optional catalytic reserve funded by the protocol or ecosystem partners. Used only when explicitly posted as claims-paying capital.
Outside scope in v1.
OmegaX Protect is intentionally bounded — built for unexpected hospital events during a defined coverage window, not general health insurance.
- 01 Chronic or pre-existing conditions
- 02 Ongoing cancer treatment, dialysis, transplant follow-up, unstable major cardiac disease
- 03 Pregnancy, maternity, fertility, or neonatal care
- 04 Routine outpatient visits
- 05 Scheduled or elective procedures
- 06 Preventive care and normal medication refills
- 07 Dental, optical, and hearing services
- 08 Ongoing mental health treatment
- 09 Evacuation, repatriation, baggage, or trip cancellation
- 10 Fraud, criminal acts, self-harm, and substance-driven events
- 11 War, sanctions, and epidemic-wide exclusions where required by policy
Non-goals for v1.
What we are explicitly not building in v1. Each of these belongs to a separate, later product path — not to this launch.
- 01 Broad annual medical insurance
- 02 Chronic-care or long-condition management
- 03 Maternity, fertility, or routine outpatient plans
- 04 Yield optimization or treasury products layered on reserves
- 05 Event-risk betting or prediction-market framing of coverage
- 06 Uncapped issuance or backdated enrollment
Keeping v1 narrow is a deliberate choice. It protects reserve integrity, keeps public language aligned with operational truth, and leaves room for broader products once claims data and capital depth support them.
Sponsors & cohorts.
Offer OmegaX Protect as a cohort benefit — conferences, team offsites, residency programs, accelerator cohorts, sponsor-backed communities.
Cohort-based enrollment
Onboard an entire cohort, team, or event community through a single sponsor-funded flow.
Sponsor-funded or subsidized
Fund protection fully or subsidize retail pricing as a member benefit. Program-specific pricing from 79 USDC at volume.
Reserve & claim reporting
Clearer view of what was funded, what was reserved, and what has been settled against the cohort.
Protocol-native visibility
Settlement state is anchored in protocol rails — not trapped in a closed operator ledger.
Launch a sponsor-backed cohort.
Talk to us about cohort pricing, subsidized enrollment, waived waiting periods, and program-specific terms. We will scope the series, cohort size, reserve floor, and activation window with you.
Business: business.omegax.health
Web app: get.omegax.health
Full FAQ.
Reference answers. For program-specific terms or sponsor cohort questions, contact the business team.
Do I need the OmegaX app?
Individuals use OmegaX to enroll, purchase protection, submit claims, and track status. Sponsor-backed cohorts can also be activated on behalf of their members.
When does coverage actually start?
Coverage begins after enrollment and the applicable waiting period. Accident cover starts after 24 hours. Illness cover starts after 7 days, unless a sponsor-configured cohort has different rules.
How many claims can I file in one window?
Each active coverage window supports one primary claim case per member in v1.
What documents will I need to submit?
Claims may require proof of enrollment, identity match, active coverage proof, hospital or clinic invoice, discharge summary or physician note, diagnostics or prescription records where relevant, and proof of payment for reimbursement top-up.
How long does a claim take?
Target decision SLAs are 24 hours for acknowledgment, 72 hours for initial review after complete evidence, and 72 hours for payout after approval. Appeals can be filed within 7 days of a decision.
Who reviews the claim?
In the current phase, OmegaX Health acts as the first claims-oracle surface with an AI claim processor producing the first-pass recommendation and a human operator backstop. The roadmap moves toward decentralized claims operators with a governance-visible dispute pathway.
What currency do payouts use?
Payouts are settled in USDC on Solana to the member’s connected wallet or payout destination.
Can a sponsor cover a team or cohort?
Yes. Sponsor-backed cohorts can enroll members, fund the reserve, and receive reporting on claim settlement. Program-specific terms and pricing are scoped with the business team.
Is it available everywhere?
Availability depends on the series, cohort structure, supported evidence formats, and launch geography. Specific regions and cohorts are announced at the time of series activation.
Is this insurance?
Protect is travel health protection with a clearly bounded scope and a fixed payout per covered event. Final program classification, licensing posture, and legal framing vary by series and jurisdiction.
Surfaces & resources.
Canonical places to go for enrollment, cohort onboarding, protocol state, and developer docs.
- → Web app — enroll, purchase, file claims · get.omegax.health
- → Business — sponsor cohort intake · business.omegax.health
- → Protocol — reserve & settlement state · protocol.omegax.health
- → Docs — technical reference · docs.omegax.health
This document is informational. Plan classification, licensing posture, and legal framing vary by series and jurisdiction. Refer to plan documentation for binding terms. Not medical advice.